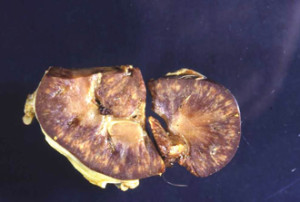
Leptospirosis in Horses
Click here to read the complete article
By Heather Thomas
Leptospirosis is a disease that can affect many species, including humans, dogs, livestock and horses. “Lepto” is caused by spiral-shaped bacteria called spirochetes. These pathogens are often found in wildlife populations, including rats and mice. The leptospires can survive in surface water, stagnant ponds, streams, or moist soil for long periods at mild temperatures. They are short-lived in cold or hot, dry weather.
Lepto is spread by discharges and secretions (especially urine) of sick and carrier animals, which often contaminate feed and water. Some infected animals, particularly with certain strains of lepto, appear to be healthy, yet harbor the bacteria in their kidneys and reproductive tract, shedding the bacteria in urine or reproductive fluids. In this carrier status they can transmit the disease to other animals even though they themselves are not sick.
Bacteria may enter a susceptible animal via the nose, mouth or eyes by contact with contaminated feed, water or urine, or through breaks in the skin on feet and legs when walking through contaminated water. Urine or contaminated water splashing into the eyes of susceptible animals can spread the disease, as can breeding. Once the leptospires enter an animal, they multiply in the liver and migrate through the bloodstream to the kidneys where they often remain; they release toxins that can damage red blood cells, liver and kidneys, especially in animals that are not an adapted host for that particular strain of leptospires.
Leptospirosis is a costly disease for the livestock and horse industry. In cattle it is a cause of infertility, delayed breeding and early embryonic death, as well as abortions or birth of premature and weak calves. Lepto is also implicated in abortions in mares. There has been an effective vaccine available for cattle, swine and dogs for many years (and therefore fewer cattle abortions from lepto), but to date there is no approved vaccine for horses.
Peggy Marsh, (Equine Medical Associates, Lexington, Kentucky) says that this disease can be a frustration for horse owners, especially when it causes abortions. It’s not always easy to determine the cause of an abortion, and if diagnostic tests point toward lepto, it’s hard to know if there will be more losses. It’s also a frustrating cause of eye problems (recurrent uveitis, originally known as moon blindness).
“Occasionally it will also cause systemic disease in horses, like it does in other species, but this is less common. This bacterium is very good at hiding in the eye, the kidney, or the uterus rather than causing systemic disease. In yearlings, however, we sometimes see kidney problems and fever, and upon investigation discover lepto as the cause,” says Marsh.
“Most of these cases respond well to antibiotic treatment, and we can clear the organism from their bodies,” she says. Most cases of leptospirosis in horses are mild, however. Occasionally we hear about a horse that gets sick from it, but severe illness is fairly uncommon. By contrast, dogs can get really sick from lepto—yet they don’t get the eye disease. Leptospirosis affects different species of animals in different ways.
Ann Dwyer DVM (Genesee Valley Equine Clinic, Scottsville, NY), has worked with many cases of leptospirosis and uveitis, and has been involved in research looking at these diseases. When horses are exposed to pathogenic strains of leptospirosis and pick up the bacteria, the resulting disease is generally mild and may not even be noticed.
“The few times I have diagnosed acute leptospirosis, the horse is just a bit off, and may have had fever for a few days, but is not very ill. If the veterinarian does a blood test, he/she might find that the horse is mildly anemic, with some minor alteration in the CBC (complete blood count), but nothing that would actually point toward leptospirosis,” says Dwyer. The few horses she has diagnosed with lepto have recovered quickly.
“If the veterinarian thinks the premises might be at risk (perhaps because of proximity to water, or cases of leptospirosis in the past, or on nearby farms), and decides to pursue some diagnostic tests, he/she could look for antibodies in the serum a few weeks after the horse was ill, or send urine samples for testing. It’s uncommon that anyone would think to do this, however, unless there was a problem on this farm already,” she says.
Horse owners often ask if lepto is contagious from horse to horse. The answer is maybe. “Early on in the disease, there probably is a short window of time when the horse may be shedding organisms in urine. It would be a minor mode of transmission, however, compared with getting the disease from wildlife on the premises. There is a theoretical possibility of transmission from horses because the infected horse may harbor leptospires in the kidneys for a short period of time—perhaps a few months. During that time there might be leptospires in the urine. On a few occasions I have submitted urine for a fluorescent antibody test to look for organisms, more for the owner’s peace of mind than anything else. I have never had this test come back positive, but some horses have been found to shed the organisms for awhile,” she says.
Dwyer feels that the incidence of leptospirosis in horses may vary from year to year, in her region. Some years are worse, and it’s generally the wetter years. The organism lives longer in the environment in moist conditions.
A person generally doesn’t have the opportunity to treat a horse when it is initially ill, because usually the disease is not recognized as leptospirosis and the horses tend to recover fairly quickly and without treatment. By the time a horse develops recurrent uveitis, the initial illness is long past.
“I have diagnosed a few lepto abortions but I don’t know what the exposure interval is for that. We do know that the ocular disease occurs many months later. Dr. Steve Roberts published clinical observations on natural disease a long time ago that suggested this. Experimental work done by Dr. Ray Morter at Purdue University in the 1960s confirmed that development of uveitis is much later,” she says.
HOPING FOR A VACCINE
There has been an effective vaccine available for cattle, swine and dogs for many years, but to date there is no approved vaccine for horses. Researchers are currently working toward an equine vaccine, but one of the biggest roadblocks is funding.
Craig Carter, DVM, Professor of Epidemiology at the University of Kentucky, has been working to build a case for an equine vaccine. “We have completed two studies. One was done by one of my graduate students, Gloria Gellin, in the College of Public Health here at the University of Kentucky. She went out to a number of horse farms and equine veterinary hospitals and collected blood samples from equine farm workers and veterinarians who have strictly equine practices. She found that many of these people were sero-positive to the leptospira organism. This study doesn’t identify exactly where or how they are getting exposed; it just shows that they have been exposed. We’d like to follow up with a similar study on people who have not been exposed to horses,” says Carter.
“There are only sporadic cases of leptosporosis diagnosed in horses around various parts of the country. Yet we are sure that many cases go undiagnosed due to inaction and lack of testing facilities. We see this disease because we often suspect it and can accurately diagnose it,” he says.
“There isn’t much in the scientific literature about the horse being a leptosporosis risk for people, but there are lots of discussions about the risks from other species. If there is zoonotic potential from horses, it might build a better case for developing an equine vaccine,” he says. Ms. Gellin presented her data at the American Public Health Association Meeting in San Francisco in October 2012.
“When I was at Texas A&M, I spent a lot of time working on canine leptosporosis, for which there is a good vaccine. I came to Kentucky in 2005. The 2006-2007 reproductive season in the equine industry here in Kentucky was one of the worst they’d had in a long time, for number of cases of lepto abortion. This was an eye-opener for me, underscored by the fact that there is no equine vaccine,” says Carter.
“As part of the study we did that year, we gathered the estimated value of the foals that were lost—on just the cases we saw here in the lab that we determined were lepto abortions. We always know that what we diagnose in the laboratory is just the tip of the iceberg. The value of the foals lost in the 2006-2007 reproductive season alone was $3.5 million. Calculating that out for a 20 year period, in which 541 cases were confirmed at this lab, it represents a very large economic loss to horse farms in Kentucky,” he says.
Carter and other researchers have spoken with several drug companies, but the drug companies don’t think there is enough market to warrant an equine vaccine. “The perception is that lepto abortion in horses only occurs in central Kentucky. So to learn if that was true, we conducted a nationwide sero-epidemiologic study in 2010-2011 that involved 30 laboratories in the U.S. and Canada. In that study we found that 45% were sero-positive for at least one leptospirosis serovar, which indicates broad exposure to leptospirosis in the horses of North America,” he explains.
A vaccine would be especially important for broodmares in preventing abortion, but would also be of interest for every horse owner. “Leptospirosis can cause severe systemic disease and death of horses, and also severe uveitis (Moon Blindness) which can lead to the loss of one or both eyes,” he says.
“My alma mater, Texas A&M, is becoming a leader in vaccine development. A lot of this work will be on the human side, but my colleagues there in the College of Veterinary Medicine have been doing some trials using a proprietary method to process antigen for vaccines. They have done an immunogenicity trial with Rhodococcus equi and have gotten good antibody and cellular immunity response, including mucosal antibodies. This is important, because the natural route of infection for R. equi is through the respiratory tree. We are hoping to conduct a similar trial for leptospirosis in the horse,” says Carter.
“If we can generate a good mucosal immunity against leptospires, this could be the best possibility for protecting the animals that are being exposed. After an immunogenicity trial, the safety and efficacy trials would come next. We are hoping we could do that work right here at the University of Kentucky,” he says.
“The first work, however, because it requires the special methods and techniques that Texas A&M is doing in developing the antigen, would be done there. If we can just come up with funding, and piggyback onto their program, this would make sense,” he says.
“We feel we have a lot of supporting data that demonstrates the need for an effective leptospirosis vaccine for horses. So we hope we can get this trial done and find another source of funding or a company that’s willing to take it the rest of the way,” says Carter.
Some horsemen who have had problems with leptospirosis have worked with their veterinarians and used the cattle vaccine off-label, and feel that it has helped prevent abortions in broodmares. The use of cattle vaccine in horses is controversial, however. “There is concern that the cattle vaccine produces a very weak immune response in horses, or might actually cause uveitis. It would be better if we had an equine vaccine,” he says.
“If we do our proposed trial at Texas A&M, we will also compare the bovine vaccine to the one we want to develop for horses. This would probably be the first thing people would ask: Why should we use or develop this when there’s a cattle vaccine that works for us? We are hoping that our trial will demonstrate that an equine vaccine would work better,” says Carter.
Dwyer says use of the cattle vaccine in horses is a controversial use. “I have a foot on either side of the fence on this question because I have occasionally used this vaccine in the past for horses,” says Dwyer.
“My impression has been that if it is used cautiously, with owner permission and education, it can help. I have used it only on horses that were sero-negative when I tested their blood to see if they have antibodies to the more common pathogenic serovars that are implicated in uveitis (L. grippotyphosa and L. pomona). I also made sure they had a normal eye exam, and were on a property that I considered high risk, meaning it was a property where multiple horses had been diagnosed with uveitis believed to be associated with leptospirosis, and risk factors such as proximity to ponds, wildlife, etc. These are the only horses that I recommend for vaccination—in the horses that were naïve to the organism,” she says.
“Then last year I gave a dose of the cattle vaccine to a horse that was in a situation like that and he reacted to the product. It wasn’t life threatening, but it was a significant local reaction where the muscle swelled up severely at the injection site and ended up with a small permanent lump,” she says.
If the vaccination can prevent abortion, however (though we don’t know that it can), or a future case of uveitis, a small blemish from the vaccine might be a small price to pay. It would all depend on the horse owner. Some owners are willing to take the risk of a possible local reaction and the use of a product that has not been tested or approved for use in horses, and others are not. They need to weigh the potential risk (which has not been quantified) when discussing the option of vaccination with their veterinarian. It would be nice to have an equine vaccine instead.